|
|
|
|
|
|
KERATOCONJUNCTIVITIS, SICCA OR DRY EYE
WHAT IS DRY EYE?
Keratoconjunctivitis sicca
(KCS) or "dry eye" describes the changes in the eye
which result from lack of tear production. To understand dry eye, it is helpful to know how tears help keep the cornea healthy. The cornea is the clear portion out front of the eye. Like all living tissue, the cornea requires a supply of oxygen and food for energy to remain healthy. Oxygen and food are supplied to most tissue by the blood that moves through the area. The healthy cornea has no blood vessel so the oxygen and food are supplied through the three layered 'tear film.'
The outer most layer of the tear film is an oily layer supplied by glands in the eyelids. This layer helps prevent evaporation of the next layer. The middle layer is the liquid (watery) layer produced by the main tear gland and a gland in the third eyelid. This is the layer where the decrease in tear production takes place. The innermost layer in direct contact with the cornea
is a layer of mucous produced by glands located in the folds of the eyelid.
The mucus layer helps the water layer remain attached to the cornea. A breakdown of the tear film by a loss of the water layer causes dry eye. This loss results in dryness to areas of the corneal surface or, in more advanced cases, drying to the entire corneal surface. When the cornea is deprived of oxygen and food through the tear film, it rapidly undergoes destructive changes.
These changes result in brown pigmentation, scar tissue growth, blood vessel growth and even ulcer development. These changes may lead to partial vision loss. The eyes of a
patient with KCS sting constantly just as ours do on a very windy day. The
stinging we feel is due to the wind drying our eyes quicker than tears can be provided. Therefore, the patient with dry eye is uncomfortable almost all the time. When a patient has dry eye, or a lack of the watery layer of the tears, the oil and mucus layer production is increased. This leads to a thick, gunky, greenish discharge that sticks to the hairs around the eye. Often this is the main reason that a patient is presented to the Veterinarian. The discharge will clear up when medication is used frequently enough but the discharge will return when the medication is stopped. When this occurs, the patient is often referred to a Veterinary Ophthalmologist for further examination and treatment.
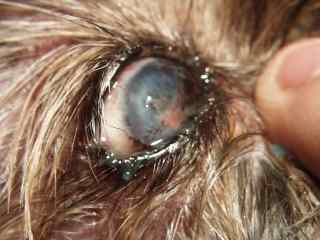
This is what a typical
patient with KCS looks like.
DIAGNOSIS OF KERATOCONJUNCTIVITIS SICCA
Diagnosis is made by determining how long the condition has been on-going, what the doctor sees when the patient is examined and a number of testing procedures. These tests include the Schirmer tear test that measures how much of the watery layer is produced in one minute. Fluorescein stain (a bright green stain) is used to define possible breaks in the corneal surface and the rate of the tear breakup. In addition, Rose Bengal stain (a reddish pink stain) may be used to evaluate the health of the outer layer of the cornea called the
epithelium. Examination of cells is sometimes recommended to define the state
of health of the conjunctiva. This test has both a prognostic and therapeutic
value.
WHAT ARE THE CAUSES OF KERATOCONJUNCTIVITIS SICCA?
A number of causes have been reported for dry eye. These include hypothyroidism, infections of the tear glands such as canine distemper virus and immune mediated diseases that attack the tear glands. Loss of nerve impulses to the gland due to longstanding ear infections will cause dry eye in some cases. Another frequent cause of dry eye is a toxic effect produced by some sulfa-containing drugs. Some of these drugs may have been given for the treatment of other diseases. It may not be possible to change the patient's medications and occasionally dry eye is treated despite being caused by other drugs. In many cases the cause of dry eye remains unknown yet treatment can still be instituted.
WHAT IS THE TREATMENT OF KERATOCONJUNCTIVITIS SICCA?
There are several considerations in treating dry eye. A prime consideration is to reduce the overgrowth of bacteria that is common in the dry eye syndrome. The dry eye patient frequently has a buildup of mucus in the folds of the eyelids that are no longer being washed with liquid tears. This mucus is food for bacterial growth. These bacteria may not be disease causing bacteria but need to be controlled. Topical antiinflammatory drugs are indicated when green stain shows no ulceration. This medication reduces inflammation and long term scarring effects. Corticosteroids (cortisone drugs) cannot be used when ulcers are present because they decrease healing speed and enhance the ulcer process. Along with antibiotics and cortisone drugs, artificial tear ointments are sometimes used to provide prolonged corneal contact overnight and during times that the patient cannot be treated frequently. Occasionally patients with a nerve loss are treated with pilocarpine given by mouth. This drug stimulates the tear gland. Unfortunately, pilocarpine may also stimulate glands all over the body. A new drug is being used for the treatment of dry eye which is tacrolimus. This drug has provided relief of symptoms in some patients while other patients have a marked increase in tear production. Unfortunately, a few patients do not respond to tacrolimus and other types of treatment are needed. Tacrolimus offers great hope for the future for our pets with dry eye.
UPDATED
It was recently reported that interferon, which is given to cats with herpesvirus, has been shown to help dogs with KCS to increase tear production. Up to 40% of dogs with KCS showed an increase in tear production when given interferon by mouth.
ARE THERE FORMS OF KERATOCONJUNCTIVITIS SICCA?
There are several forms of the dry eye syndrome that we commonly diagnose. These include: Partial dry eye that results from a slight reduction of tear production. Intermittent dry eye is the result of temporary loss of tear production followed by periods of normal production. Complete dry eye is the complete absence of tear secretion. Finally, temporary dry eye is the short
term loss of tear production due to a variety of causes such as
anesthesia.
WHAT IS THE EVENTUAL OUTCOME OF A PATIENT WITH KCS?
Most patients with dry eye will do well if medications are administered on a timely basis. In cases where medicines cannot be given regularly or do not work, surgical techniques must be considered. A parotid duct transposition or PDT (surgical movement of a duct from a saliva producing gland to the eye) is available. The PDT is needed in patients who have had no response to medication or who responded well initially and then had a relapse. In general, with consistent treatment, no patient need
lose eyesight due to the dry eye condition.
| |