|
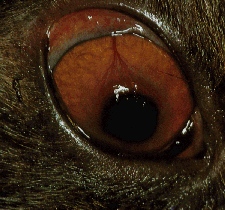
Feline Corneal Sequestrum
Wat corneal sequestrum is a condition peculiar to the cat where corneal stromal necrosis occurs.
The dead stroma becomes pigmented and in most cases the plaque extrudes and sloughs leaving a corneal ulcer with a pigmented crater. Various names have been given to this lesion since it first description in 1965. These include corneal mummification, the isolated black lesion, corneal nigrum, keratitis nigrum, focal degeneration of the cornea, corneal necrosis, primary necrotising keratitis and corneal sequestration or sequestrum.
The cause of the corneal necrosis is unknown. Some authors suggest a primary corneal dystrophy, while others suggest that the necrosis is secondary to a plethora of factors which make the cornea vulnerable. The origin of the black discolouration of the desiccated stroma is thought to be epinephrine products in the tears which adsorbs into the degenerative stroma.
Incidence of Corneal Sequestrum by Breed
- Himalayan 35%
- Persian 35%
- Siamese 15%
- Abbysinian 5%
- Domestic 10%
Corneal sequestra are seen in cats of all ages except the neonate, but most tend to be young adults. There is no sex predilection, but there is a noticeable breed distribution.
The Persian, Siamese and Himalayan are over represented, but cases also occur with lesser frequency in the Domestic Shorthair breeds. This breed predisposition may not be of direct genetic origin, as these breeds share certain conformational factors which in turn may predispose to corneal sequestration. These breeds are relatively exophthalmic, and as such are subject to additional risk of trauma. In addition, some of these cats have lagophthalmos, and the tear film is not spread adequately over the axial cornea which results in drying. Also many affected cats have subtle medial lower lid entropion which may chronically irritate the cornea.
The usual clinical presentation is a cat with a history of hronic ocular signs. Most affected cats exhibit blepharospasm, lacrimation and protrusion of the third eyelid. The lesion is a dark brown to black plaque which is oval or round and often raised above the corneal surface. Application of fluorescein dye to the cornea often reveals dye retention around the periphery of the lesion, but the sequestrum itself does not stain. Sequestra are usually axial (in the center of the cornea), but may be paraxial (off-center). Cats are usually presented with unilateral signs, but bilateral cases occur not infrequently. The cornea around the sequestrum is vascularized to varying degrees.
The vascularization is usually superficial and there is often corneal edema and stromal cellular infiltration as a foreign body reaction to the necrotic tissue occurs.
Some cases are presented where the opacity is confined to the stroma, and such a patient may not show signs of discomfort. These are thought to be earlier lesions, or perhaps this results following sloughing or surgical removal, and subsequent healing and re- epithelialization, of more superficial sequestra.
These sequestra often progress, become more dense, acquire distinct borders, separate from the adjacent and underlying stroma and begin the process of extrusion with loss of the overlying corneal epithelium. Some authors classify the sequestrum which is darker and extruding as a Type I sequestrum, while the lighter brown or amber lesion which is covered by an intact but degenerate epithelium as a Type II lesion. Other authors feel that they are both different stages of the same disease process. The classification is helpful as Type I lesions often require surgery whereas Type II lesions may be handled surgically or conservatively and reassessed at a later time.
Histologic examination of keratectomy specimens from cats with corneal sequestrum characteristically reveals coagulation necrosis of the corneal stroma. The overlying epithelium is usually absent, but if present is also necrotic. Early sequestra are characterized by degenerative corneal epithelium, normal and degenerative fibroblasts and keratocytes, amorphous cellular debris, inflammatory cells and disorganized stromal fibrils.
Older sequestra are characterized by complete degeneration of fibroblasts, collagen fibrils and epithelium. Most of the vascularization and inflammatory cells are located in the periphery and base of the desiccated stroma. The predominate cells are lymphocytes and plasma cells, with occasional neutrophils, macrophages and giant cells. The general histologic picture is that of a foreign body type reaction to the necrotic tissue. Periodic Acid Schiff staining of keratectomy specimens reveals PAS positive granules in adjacent keratocytes which on EM are dense membrane bound lysosomal structures.
The significance of these structures is not known. Occasional groups of gram + cocci (micrococci) and fungal hyphae are seen in the necrotic stroma. Cultures taken from the posterior surface of the sequestrum have yielded Micrococci, Staphylococci, Streptococci, Moraxella and Aerobacter spp. These bacteria may initiate the primary process of corneal sequestrum, but in all probability are secondary invaders.
The treatment of corneal sequestrum in the cat varies considerably between surgeons. Some adopt a conservative approach and allow the sequestrum to slough while treating with antibiotics and ocular lubricants. Extrusion may take months to years, and thus therapy and ocular pain may be prolonged. The main advantage to surgical excision of sequestra is significant shortening of the course of the disease.
Superficial sequestra may be treated by superficial keratectomy. The cornea in the cat is approximately 0.6 mm in thickness, and some surgeons recommend that dissection in the cornea beyond 0.3 mm is risky. Once the surgeon has removed as much of the sequestrum as he or she feels comfortable, the cornea must be supported while it heals. Post surgically, small superficial sequestra may only require topical antibiotic and ocular lubricant to result in satisfactory healing. Some superficial sequestra may be supported post-surgically with a Therapeutic soft contact lens.
Other surgeons may elect to support such corneas with a nictitans flap for ten to fourteen days. Sequestra which require deeper dissection in the cornea may require the placement of a conjunctival graft for support. Techniques are described for advancement grafts, pedicle grafts, and bridge grafts. In occasional cases a pedicle graft may remain vascularized even after resection of the pedicle. Blogg et al advocate a permanent pedicle graft which eliminates the need for a second graft release procedure. Deep sequestra may be supported with a corneal scleral transposition procedure. It is my experience that the visual axis may be best preserved with this procedure.
Post surgical medical management involves topical antibiotics, acetylcysteine, atropine and ocular lubricants. An elizabethan collar to prevent self trauma is mandatory. Once the cornea has re-epithelialized, some surgeons recommend the use of topical anti-inflammatory medications to reduce fibroplasia and subsequent scarring. Caution is required however, as some cats with sequestrum are positive for feline herpesvirus, and topical steroid may incite reactivation of latent herpesvirus infection.
A polymerase chain reaction (PCR) test for feline herpesvirus is recommended for cats with corneal sequestrum.
| |